Heart Diseases and Their Treatments: What You Need to Know
Introduction
Have you ever felt a sudden tightness in your chest or noticed a family member becoming breathless after a simple walk? Heart issues can sometimes sneak up without much warning, but they don't have to be a life sentence. This World Heart Day, take a moment to explore the common heart ailments that affect millions and the treatment modalities that can make a real difference. Whether you are a doctor guiding your patients or someone looking for information to help a loved one, our guide will walk you through everything you need to know about keeping the heart healthy and strong.
Understanding Common Heart Ailments
Heart ailments can manifest in many forms, affecting the heart's ability to function properly. Some of the most common heart diseases include:
Coronary Artery Disease (CAD): This occurs when the arteries that supply blood to the heart muscle become narrowed due to cholesterol build-up. It often leads to chest pain, shortness of breath, and even heart attacks.
Arrhythmias: This is an irregular heartbeat, where the heart may beat too fast, too slow, or in an erratic manner. It can lead to palpitations, dizziness, and in severe cases, sudden cardiac arrest.
Heart Valve Diseases: Valve diseases occur when the heart valves do not open or close properly, disrupting blood flow and straining the heart.
Heart Failure: This does not mean the heart has stopped working. Instead it means that it is not pumping blood as efficiently as it should. It can be a result of various underlying conditions, including CAD, high blood pressure, and diabetes.
Congenital Heart Diseases: These are structural issues with the heart that are present from birth. They can affect the walls, valves, or blood vessels of the heart and vary in severity.
The Role of Medical Interventions in Treating Heart Ailments
While lifestyle changes and medications can help manage some heart conditions, others require interventional procedures. Let's explore some of the key interventional procedures for heart ailments:
- Angioplasty for Coronary Artery Disease
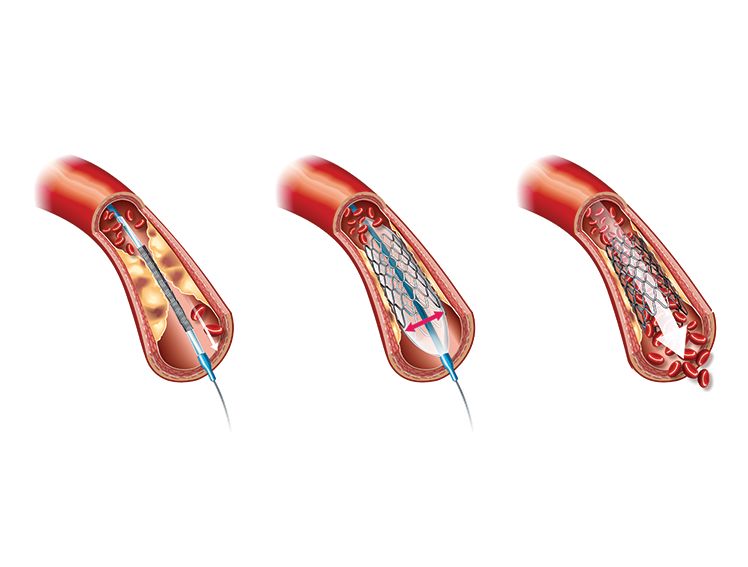
One of the most common treatments for Coronary Artery Disease is angioplasty. When an artery is blocked or narrowed, a tiny mesh tube called a stent is inserted into the artery to keep it open. This procedure is known as angioplasty.
How It Works: During angioplasty, a balloon is inflated inside the blocked artery in order to widen it. Once the artery is widened, a stent is placed to keep it open and ensure proper blood flow.
Benefits: Stents significantly reduce the risk of heart attacks and help in relieving symptoms like chest pain and breathlessness. Patients typically recover quickly and can resume normal activities within a few days.
- Heart Valve Replacement
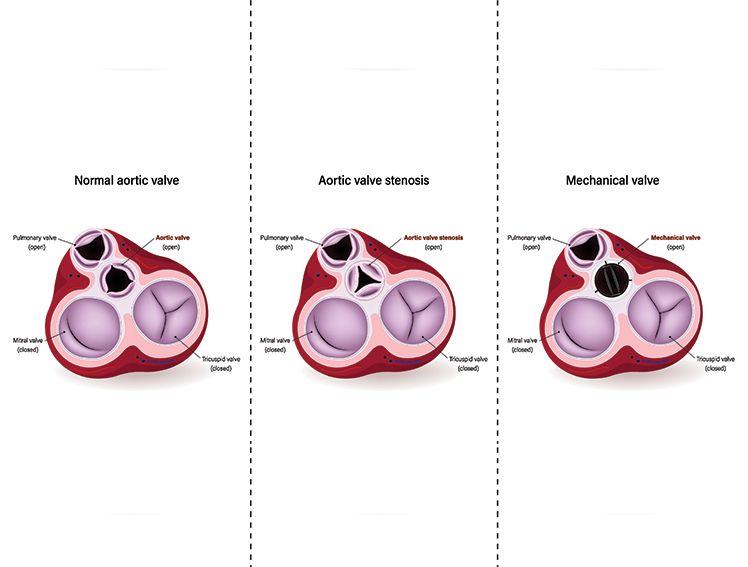
Heart valve problems like stenosis (narrowing) or regurgitation (leakage), often require repair or replacement. Valve replacement is an effective treatment that can restore normal blood flow and improve the heart's function.
Types of Valve treatment:
- Valve Repair: This involves fixing the existing valve without replacing it. Techniques can include reshaping the valve, removing excess tissue, or repairing holes.
- Valve Replacement: When the damage is too severe for repair, the valve is replaced majorly in the case of Aortic stenosis either surgically or through a minimally invasive procedure known as Transcatheter Aortic Valve Implantation/ Replacement (TAVI/TAVR).
Benefits: Valve repair or replacement can improve the quality of life by alleviating symptoms like fatigue and shortness of breath. It also prevents complications such as heart failure or stroke.
- Coronary Artery Bypass Grafting (CABG)
CABG, commonly known as bypass surgery, is a procedure that creates a new pathway around blocked arteries to improve blood flow to the heart. It is often recommended for patients with multiple blocked arteries or severe CAD.
How It Works: A healthy blood vessel, normally taken from the leg or chest, is grafted to bypass the blocked coronary arteries. This lets the blood to flow freely to the heart muscle.
Benefits: Bypass surgery can significantly reduce the risk of heart attacks, alleviate chest pain, and improve overall heart function. Recovery may take a few weeks to months, but the long-term outcomes are generally positive.
- Pacemaker Implantation for Arrhythmias
Arrhythmias, or irregular heartbeats, can be life-threatening if not treated. A pacemaker is a small device placed in the chest to help control abnormal heart rhythms.
How It Works: The pacemaker sends electrical signals to the heart to help it beat regularly and at a proper rate. It is implanted through a minimally invasive procedure.
Benefits: Pacemaker implantation can prevent complications associated with arrhythmias, such as stroke or sudden cardiac arrest. It allows patients to lead a normal and active life with regular follow-ups.
- Heart Transplant for Severe Heart Failure
For patients with severe heart failure where other treatments have not worked, a heart transplant may be the last option. It involves replacing the diseased heart with a healthy heart from a deceased donor.
How It Works: The diseased heart is removed, and a donor heart is surgically implanted. The procedure is complex and requires a highly skilled team of surgeons.
Benefits: Heart transplants offer a new lease on life for many patients, improving survival rates and quality of life. Post-transplant care is crucial to prevent rejection and infections.
Recovering from Heart Procedures
Recovery from heart procedures varies depending on the type of treatment, the patient’s overall health, and how well they follow post-operative care instructions. Here are some general tips for a smoother recovery:
Follow Your Doctor’s Advice: Attend follow-up appointments and take prescribed medications as directed. Regular check-ups are crucial for monitoring progress and making any necessary adjustments to treatment plans.
Adopt a Heart-Healthy Lifestyle: Incorporate a balanced diet rich in fruits, vegetables, whole grains, and lean proteins. Avoid smoking, limit alcohol consumption, and manage stress through meditation, yoga, or other relaxation techniques.
Stay Active: Engage in light physical activities like walking, as recommended by your doctor. Cardiac rehabilitation programs can provide structured exercise routines tailored to your recovery needs.
Listen to Your Body: It’s important to rest when needed and not push yourself too hard. Overexertion can slow down the healing process.
How is Meril Empowering Doctors with Advanced Solutions for the treatment of Heart
Meril is at the forefront of supporting doctors in the treatment of heart diseases by providing innovative and advanced solutions like latest Drug Eluting Stents, dissolving stents known as BioResorbable Scaffolds, minimally invasive and surgical heart valves, and surgical products. With its cutting-edge ranges of stents, Meril helps cardiologists effectively manage Coronary Artery Disease (CAD). These stents are designed with ultra-thin struts and drug coatings, offering flexibility and reducing the chances of restenosis.
Meril offers a complete portfolio for Metal Less PCI, a technology that eliminates the need for permanent metal implants in the arteries. This procedure uses BioResorbable scaffolds, which naturally dissolve over time, leaving no foreign material in the body. This reduces long-term complications such as inflammation or scarring, and allows the artery to restore its natural movement and function. This allows doctors to perform minimally invasive procedures with greater precision and improved patient outcomes, leading to faster recovery and fewer complications.
Additionally, Meril's drug-coated balloons, such as the MOZEC PEB, deliver targeted doses of paclitaxel to the affected areas, minimising tissue proliferation and reducing the risk of restenosis in peripheral arteries. These balloons allow for an efficient, non-stenting solution that combines the benefits of angioplasty with drug delivery, improving treatment outcomes in patients with peripheral artery disease.
For heart valve replacement, Meril's products are helping transform the way doctors treat severe aortic stenosis, especially in high-risk patients who are not ideal candidates for traditional open-heart surgery. By providing an option for valve replacement without open surgery, Meril enables interventional cardiologists to offer safer, less invasive alternatives that significantly reduce recovery time. Additionally, Meril’s comprehensive range of surgical products, including specialised heart valves and sutures, further supports cardiac surgeons by enhancing the efficiency and success rates of heart procedures. This commitment to innovation and quality empowers doctors to deliver the best care possible to their patients.
Conclusion
As we observe World Heart Day, it is important to remember that heart diseases are manageable. If you or a loved one is experiencing symptoms related to heart conditions, consult a healthcare professional for proper evaluation and guidance.
FAQs
References
https://www.mayoclinic.org/diseases-conditions/coronary-artery-disease/symptoms-causes/syc-20350613#:~:text=Coronary%20artery%20disease%2C%20also%20called,are%20almost%20always%20to%20blame.
https://www.mayoclinic.org/diseases-conditions/heart-arrhythmia/symptoms-causes/syc-20350668
https://my.clevelandclinic.org/health/diseases/17639-what-you-need-to-know-heart-valve-disease
https://www.heart.org/en/health-topics/heart-failure/what-is-heart-failure
https://my.clevelandclinic.org/health/diseases/21674-congenital-heart-disease
https://www.mountsinai.org/health-library/discharge-instructions/angioplasty-and-stent-heart-discharge#:~:text=a%20coronary%20artery.-,A%20coronary%20artery%20stent%20is%20a%20small%2C%20metal%20mesh%20tube,coronary%20artery%20that%20is%20blocked.
https://www.mayoclinic.org/tests-procedures/heart-valve-surgery/about/pac-20384901
https://www.nhs.uk/conditions/coronary-artery-bypass-graft-cabg/#:~:text=A%20coronary%20artery%20bypass%20graft,oxygen%20supply%20to%20the%20heart.
https://my.clevelandclinic.org/health/treatments/17360-permanent-pacemaker