Fistula Types & Treatments: From Anal to Obstetric Interventions
Introduction
Fistulas can develop in various parts of the body and arise from different causes. Understanding the various types of fistulas and their treatment options can have a profound impact on the lives of those affected. Two types that often come up are anal fistulas and obstetric fistulas, and each needs its own kind of care.
A fistula happens when an unusual connection forms between two body parts that generally don’t connect. This can lead to leakage, discomfort, and infections if left untreated. Understanding the type of fistula is crucial for selecting the proper treatment and improving one's everyday life.
What Exactly Is a Fistula? Common Types Explained
At its core, a fistula is an abnormal connection, or tunnel, between organs or tissues. This typically occurs due to infection, injury, or complications during childbirth. The main kinds include:
Anal fistula: A small channel that connects the inside of the anus to the skin around it. It often results from infections in nearby glands.
Obstetric fistula: This develops mainly after long, difficult labour, creating a passage between the vagina and bladder or rectum. It causes unwanted leakage and poses a significant health issue in certain areas.
Recognising these types can help people notice symptoms early and seek appropriate care.
Signs of Obstetric Fistula to Watch For
Obstetric fistula can cause distressing symptoms, such as:
Uncontrolled leakage of urine or stool through the vagina.
Pain or discomfort in the pelvic area.
Repeated infections or irritation near the genital region.
Emotional challenges from social isolation.
Anyone noticing these signs should consider seeing a healthcare professional to explore treatment possibilities.
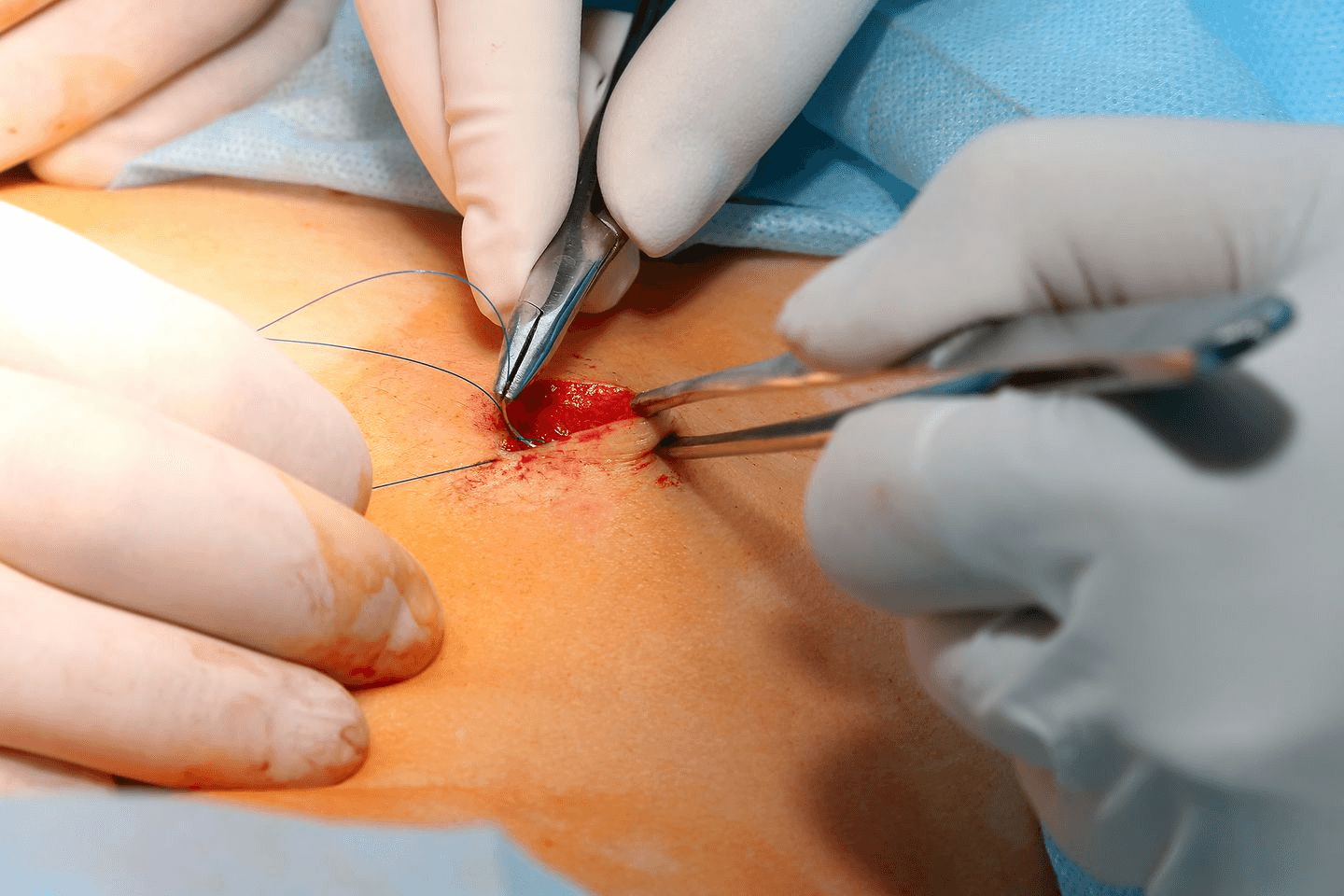
Anal Fistula and How Surgery Helps
An anal fistula usually starts after an abscess near the anus doesn’t heal properly. It can cause pain, swelling, and discharge. Doctors typically diagnose it through examination and, in some cases, imaging.
Treating an anal fistula often means surgery to remove infected tissue and close the abnormal connection. Surgeons must strive to preserve the muscles controlling bowel movements to prevent issues such as leakage.
What Happens During Anal Fistula Surgery?
Surgery aims to:
Remove unhealthy tissue causing infection.
Close the fistula tunnel to prevent it from reopening.
Protect the anal sphincter muscles to keep control over bowel movements.
Different surgical options exist depending on the fistula’s complexity, including seton placement or flap repairs, which help healing while protecting muscle function.
Fistula Care, Healing, and Long-Term Recovery
Fistula treatment is not just about the procedure. Healing well and preventing complications require consistent care before and after surgery. Whether it’s anal fistula surgery or treatment for an obstetric fistula, long-term recovery plays a major role in overall outcomes.
Why Early Attention Matters
Getting help when symptoms begin, like leakage, pain, or irritation, can prevent a fistula from becoming more complex. Early recognition of symptoms of obstetric fistula or anal fistula allows timely evaluation and smoother recovery.
Healing and Recovery: What Usually Supports Better Outcomes
Recovery depends on several factors, including the type of fistula, the approach used, and general health. Many people benefit from:
Gentle hygiene habits to avoid irritation
Balanced meals that support healing
Gradual physical movement as guided
Regular follow-ups to monitor progress
Emotional support for stress and comfort
These habits help the body heal naturally and avoid additional strain on the fistula site.
Lifestyle Adjustments After Fistula Surgery
Making mindful changes after fistula surgery, especially for anal fistulas, can support comfort and recovery:
Staying hydrated helps maintain soft stools
Eating fibre-rich foods reduces straining
Avoiding long sitting hours eases pressure
Practising pelvic health exercises when suitable
Seeking help for discomfort instead of ignoring it
These day-to-day steps can ease healing and reduce the risk of symptoms returning.
The Bigger Picture: Long-Term Wellbeing
Both anal fistula and obstetric fistula can affect quality of life, but with timely care, the right procedure, and good after-care, many people experience improvement. While treatment helps correct the abnormal connection, long-term wellness relies on healthy habits, emotional support, and regular medical follow-ups.
Conclusion
Fistulas, whether anal or obstetric, can deeply impact daily life, but understanding their causes, symptoms, and treatment options empowers people to seek help early. Anal fistulas often arise from infections, while obstetric fistulas are usually linked to childbirth complications. Both require specialised care, and timely attention can make treatment smoother.
While fistula surgery plays a key role in closing the abnormal connection, long-term healing depends on good hygiene, supportive habits, and ongoing follow-ups. With better awareness, early recognition, and the right care approach, individuals can manage symptoms more comfortably and work toward improved well-being.