Hiatal Hernia: Symptoms, Diagnosis, and Treatment Options
Introduction
You finish a heavy meal and, within an hour, feel a burning sensation in your chest. You try to sit upright, sip some water, and hope it settles. It happens again after a few days, especially after eating late or lying down too soon. You might dismiss it as “just acidity".
But in some cases, repeated heartburn like this can be linked to a condition called a hiatal hernia. The name sounds technical, yet the problem itself is fairly straightforward and easier to understand than it seems.
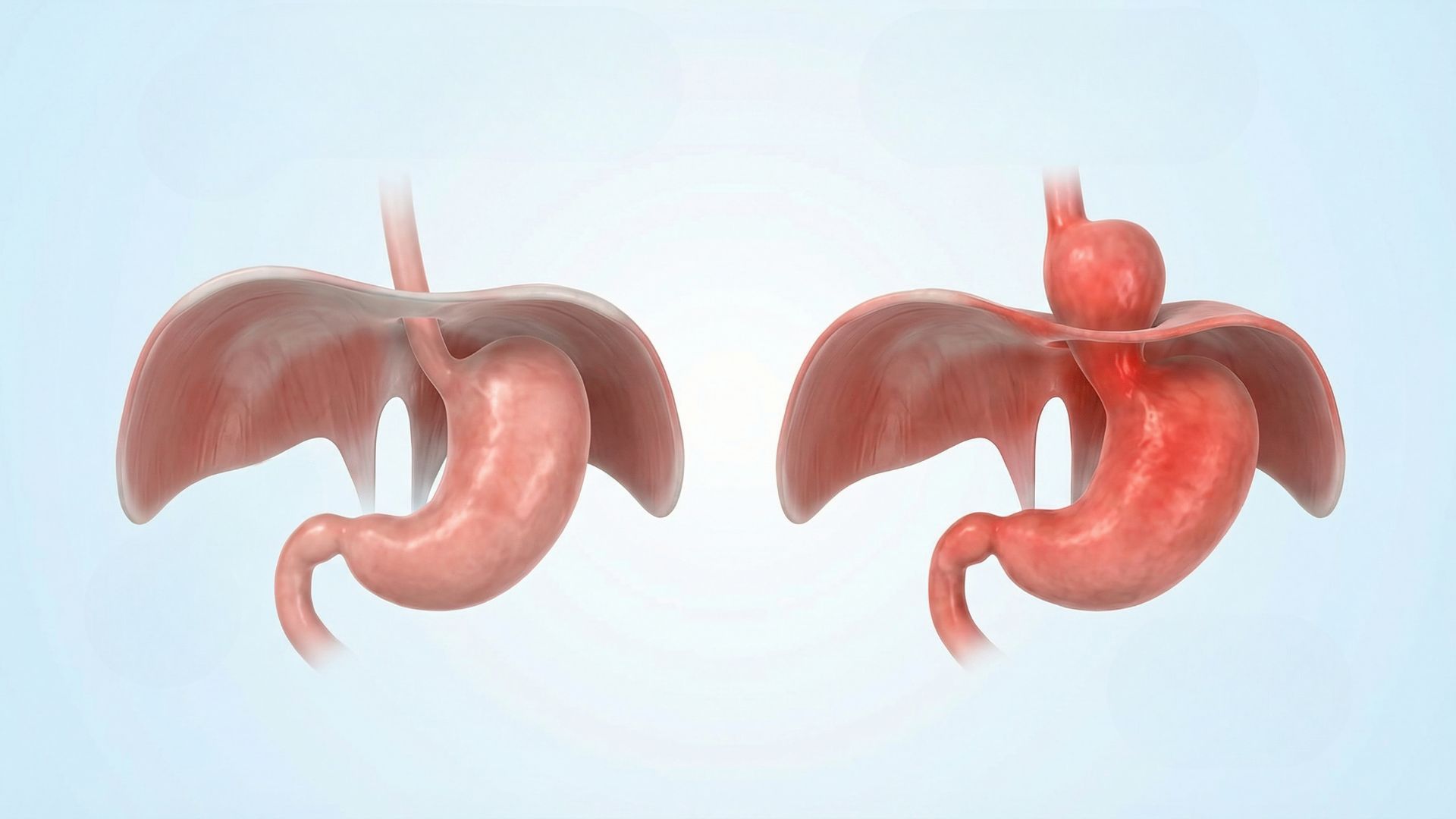
A hiatal hernia happens when a part of your stomach moves upward into your chest through an opening in the diaphragm. For some people, it causes no symptoms at all. For others, it can lead to discomfort, acid reflux, and complications if left untreated.
In this blog, we will walk you through what a hiatal hernia is, its symptoms, how it is diagnosed, and the available treatment options, so you can better understand what may be happening inside your body.
What Is a Hiatal Hernia?
To understand a hiatal hernia, it helps to know a little basic anatomy.
Your diaphragm is a large muscle that separates your chest from your abdomen. It plays a major role in breathing. There is a small opening in the diaphragm called the hiatus, through which the food pipe (oesophagus) passes before connecting to the stomach.
In a hiatal hernia:
The top part of the stomach pushes upward
It moves through the hiatus
It enters the chest cavity
A small hiatal hernia may not cause noticeable problems. In fact, many people discover they have one incidentally during a scan or endoscopy done for another reason.
However, larger hernias can interfere with the normal functioning of the lower oesophageal sphincter (the valve that prevents acid from flowing back up), leading to reflux symptoms.
Types of Hiatal Hernia
Hiatal hernias are broadly divided into four types:
Type 1: Sliding Hiatal Hernia
It is the most common type, accounting for about 90–95% of cases.[1]
The junction where the food pipe meets the stomach slides upward into the chest.
It may move up and down.
It is often associated with acid reflux.
Most people diagnosed with a hiatal hernia have this type.
Type 2: Paraesophageal Hernia
In this type:
Part of the stomach pushes through the hiatus
It sits beside the oesophagus
The gastro-oesophageal junction remains in its normal position
Though less common, this type can pose a greater risk because part of the stomach can become trapped.
Type 3: Mixed Hernia
It is a combination of Type 1 and Type 2 features. Both the junction and a portion of the stomach move upward.
Type 4: Complex Hernia
It is rare and more serious. Along with the stomach, other abdominal organs, such as the intestines or spleen, may move into the chest cavity.
Common Symptoms and Causes of Hiatal Hernia
Not everyone with a hiatal hernia has all symptoms. When symptoms do occur, they are often related to acid reflux.
Common Symptoms
Heartburn (burning sensation in the chest)
Regurgitation of food or sour liquid
Difficulty swallowing
Chest discomfort
Bloating after meals
Chronic cough or throat irritation
For example, if you notice a burning sensation in your chest after eating spicy food or after lying down soon after dinner, it could be due to reflux worsened by a hiatal hernia.
In more severe cases (especially paraesophageal hernias), symptoms may include:
Severe chest pain
Vomiting
Difficulty swallowing solids
Shortness of breath
Causes and Risk Factors
Hiatal hernias may develop due to:
Age-related weakening of the diaphragm muscles
Increased pressure inside the abdomen (obesity, pregnancy)
Chronic coughing
Heavy lifting
Constipation and straining
Smoking
Previous abdominal injury or surgery
The condition usually develops slowly over many years.
Diagnosis and Tests Of Hiatal Hernias
If you experience persistent reflux symptoms, your doctor may suggest tests to confirm the diagnosis and rule out other conditions.
1. Upper Endoscopy
A fine, flexible tube with a camera is passed into your mouth, into the oesophagus, and into the stomach. With this test, the doctor can:
Detect inflammation
Identify ulcers
Rule out tumours
Confirm the presence of a hernia
2. Barium Swallow (Oesophageal)
You swallow a contrast liquid, and X-rays are taken. This test shows:
The size of the hernia
The position of the stomach
Structural abnormalities
3. Oesophageal Manometry
This measures the pressure and movement of your oesophagus. It helps rule out motility disorders that may mimic reflux.
4. 24-Hour pH Monitoring
This test measures how much acid enters the oesophagus over a day. It is often considered the gold standard for confirming acid reflux. Accurate diagnosis is important because treatment decisions depend on both symptoms and the type of hernia.
Management and Treatment Options of Hiatal Hernias
Treatment depends on:
- Type of hernia
- Severity of symptoms
- Presence of complications
1. Medications
For many patients with hiatal hernias, medications are the first line of treatment.
- Antacids for quick relief
- H2 blockers to reduce acid production
- Proton Pump Inhibitors (PPIs) to control persistent acid reflux
These help relieve symptoms but do not correct the hernia itself.
2. Surgical Treatment
Surgery may be recommended if:
- Symptoms do not improve with medication
- There are complications (bleeding, obstruction, strangulation)
- A large paraesophageal hernia is present
The most common procedure is laparoscopic hiatal hernia repair, often combined with fundoplication to prevent reflux.[2]
During surgical repair, surgeons use advanced fixation and reinforcement materials to support tissue healing. Solutions such as Filaprop, a polypropylene suture from Meril, may be used to achieve secure, reliable tissue approximation during abdominal procedures. Proper fixation plays a key role in ensuring durability and reducing the risk of recurrence.
Surgery is generally minimally invasive and associated with shorter recovery times when performed laparoscopically.
Lifestyle and Home Management for Hiatal Hernias
Many patients can control symptoms effectively through lifestyle adjustments.
Practical Measures
Eat smaller, more frequent meals
Avoid lying down immediately after eating
Maintain a healthy body weight
Elevate the head of your bed with pillows by 6–8 inches
Avoid trigger foods (spicy, fatty, acidic foods)
Limit caffeine and alcohol
Stop smoking
For instance, if you typically eat dinner at 10 PM and go to bed at 10:30 PM, simply shifting dinner earlier may significantly reduce nighttime reflux.
Lifestyle measures are especially helpful in sliding hiatal hernias.
When to See Your Doctor for Hiatal Hernias?
You should consult a doctor if you experience:
Persistent heartburn not relieved by medication
Difficulty swallowing
Unexplained weight loss
Vomiting blood
Black stools
Severe chest pain
While heartburn is common, persistent or worsening symptoms require evaluation to prevent complications such as esophagitis or Barrett's oesophagus. If you have sudden, severe chest or abdominal pain along with vomiting, seek emergency care immediately. This may indicate a trapped or strangulated hernia.
Conclusion
A hiatal hernia becomes common as people age. In many cases, it causes little to no trouble. However, when symptoms like acid reflux become persistent, proper evaluation and management are necessary.
The good news is that most cases can be managed effectively with medication and lifestyle changes. Surgery is reserved for more severe or complicated cases and is typically safe and minimally invasive when indicated.
Understanding your symptoms and seeking timely medical advice can help to prevent long-term complications and improve your quality of life.