Things to Know About Intrauterine Devices
What is an Intrauterine Device?
An intrauterine device (IUD) is a birth control device inserted into the uterus to prevent pregnancy by a trained or specialised medical professional. It is a small T-shaped plastic device. It is a long-acting reversible contraception (LARC), which means it can prevent pregnancy for many years, i.e., up to 10 years, depending on the type of IUD. It is also a reversible form of birth control, meaning that your healthcare provider can remove it if you decide to get pregnant at any point.
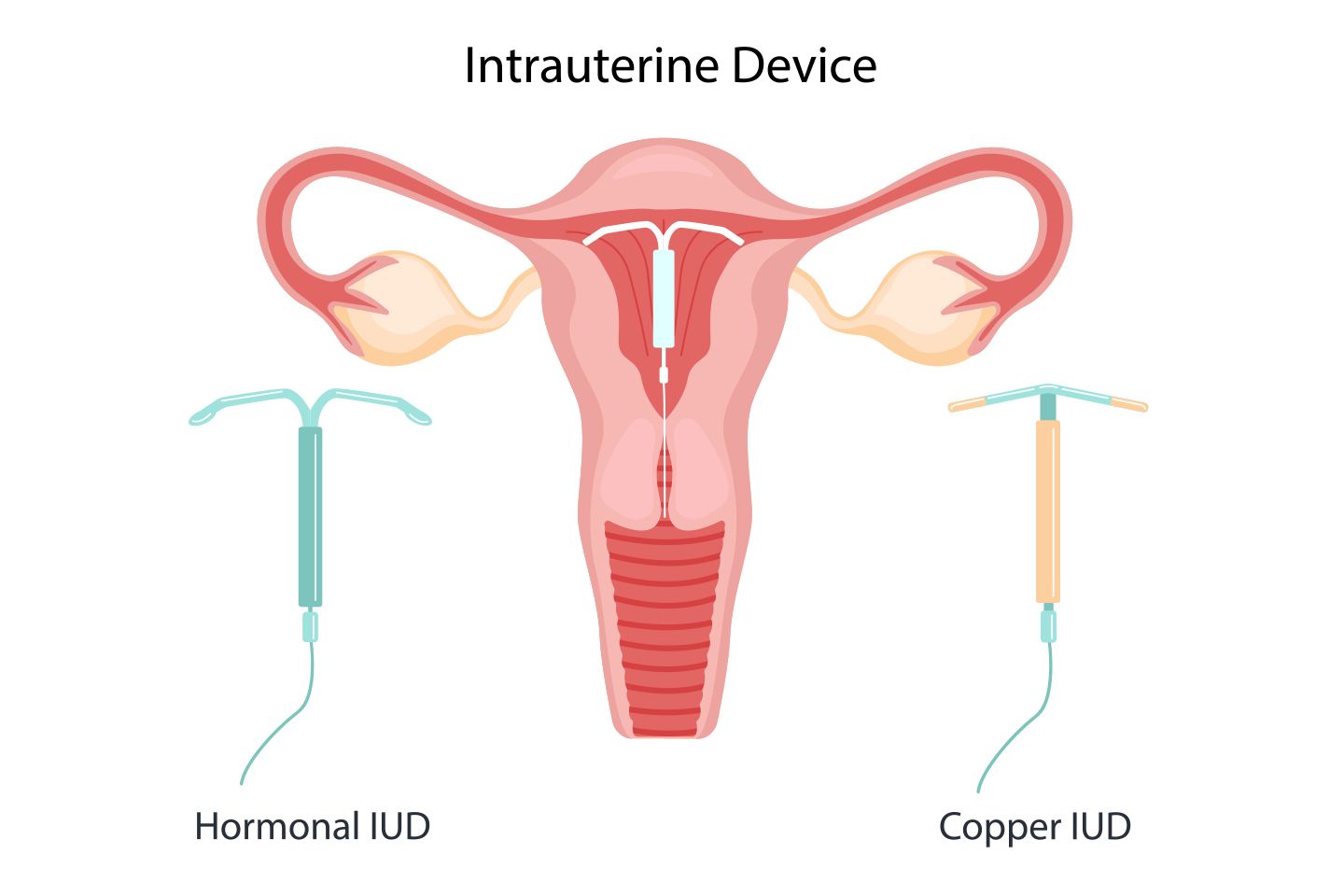
Types of IUDs
There are two main types of IUD devices: copper and hormonal. They both prevent pregnancy by keeping the sperm from reaching the egg and fertilising it. They are also equally effective at preventing pregnancy, with more than 99% effectiveness.
- Copper IUD (Cu-IUD): Copper intrauterine contraceptive device releases copper into the uterus, which releases copper ions locally and changes the makeup of the uterine lining and the cervical mucus. The release of the copper ions also amplifies the inflammatory response in the region. This causes the endometrium, or uterine lining, to become inflamed, making it difficult for sperm to survive in the fallopian tubes and reach the eggs. If at all the fertilization takes place, then the fertilised egg cannot implant itself.
- Hormonal IUD (HIUS): As for hormonal intrauterine devices, they release the progestin hormone levonorgestrel (LNG) into the body to help prevent pregnancy. Progestin is like the hormone progesterone that is naturally found in the body. When released into the uterus, levonorgestrel thickens the cervical mucus, making it tougher for sperm to move through it and reach the egg. It also thins out the uterine lining, which makes it tougher to produce and fertilise eggs.
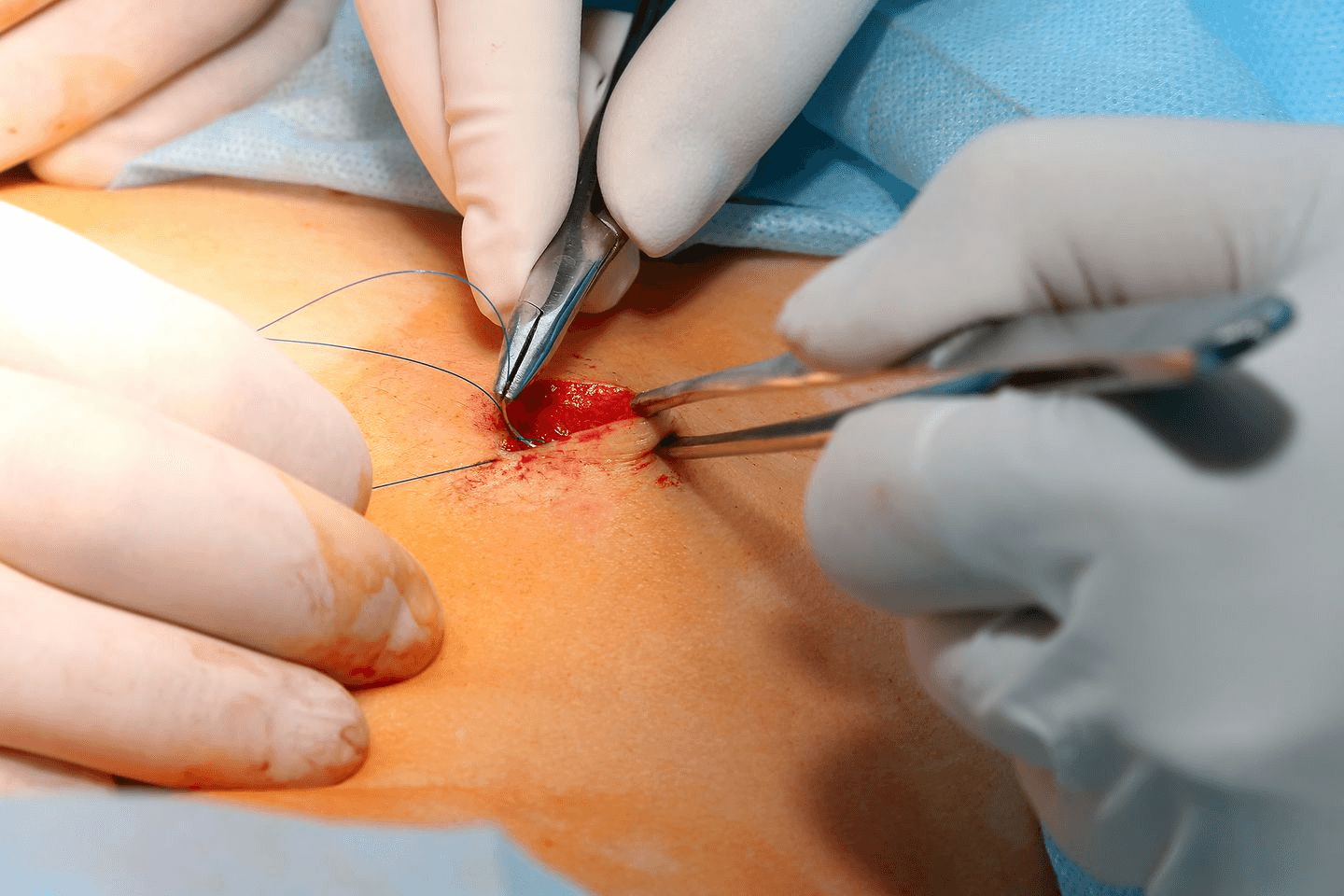
IUD insertion
Intrauterine devices must only be inserted, adjusted, and monitored by a trained healthcare provider. The process is not long and can be done easily at your doctor’s clinic. After cleaning the area, your healthcare provider will position you on a table as if you were receiving a pap smear —on stirrups with knees bent and legs open and then insert a speculum into your vagina to help widen your vaginal opening and make room for the IUD.
Next, they will slide a tube encapsulating the IUD through the vagina and into the uterus and push it inside the uterus. They will then remove the tube, leaving two strings dangling outside the cervix but inside the vaginal cavity. Not only are these strings used to pull the IUD out of the uterus when needed, but they also help to check if it is in the proper position.
Contraindications
You may have to get tested for sexually transmitted infections (STIs) and take a pregnancy test before inserting the IUD. This is because IUDs cannot be administered to individuals who:
- Are pregnant
- Are at elevated risk for contracting STIs (sexually transmitted infections)
- Have an active STI
- Have cervical or uterine cancer, and
- Are experiencing unexplained vaginal bleeding
People allergic to copper or suffering from Wilson’s disease should avoid using copper IUDs, and people with severe liver disease or breast cancer should avoid using hormonal IUDs.
Advantages of intrauterine devices
- It is a long-acting reversible contraception (LARC).
- It is effective immediately upon insertion, preventing pregnancy for many years, i.e., up to 10 years, based on the type of IUD chosen.
- It is safe to use for breastfeeding individuals.
- Other medications do not impact their effects.
- Some hormonal IUDs can reduce heavy menstrual bleeding and relieve menstrual cramps and pain from endometriosis.
- Copper IUDs are an effective form of emergency contraception.
Side effects of the intrauterine device
You may experience different symptoms based on the type of IUD you choose. The potential side effects of hormonal IUDs include:
- Irregular periods or amenorrhea
- Headaches, acne, and breast tenderness
- Mood changes
- No protection against STIs
- Small fluid-filled cysts on the ovaries, which usually disappear in a few weeks without treatment.
As for copper IUDs, some people may experience heavier bleeding and more cramps during their periods when using them. However, this usually only lasts for the first few months after getting the IUD. Your periods should lighten after a few months of insertion.
Copper IUDs can also have side effects such as:
- Unexpected vaginal discharge
- Backaches
- Spotting between periods
The IUD insertion process can cause discomfort and pain for some women. Other potential symptoms that women can experience during and after IUD insertion are:
- Cramps and pain
- Dizziness or light-headedness
- Back pain
Potential health risks of the intrauterine device
While these are rare since IUDs are safe and effective, there are a handful of potential health risks to look out for, including:
- Pelvic infections
- Perforation of the womb
- Expulsion or displacement of IUD
- In case you do get pregnant, you are likely to see a high-risk pregnancy or ectopic pregnancy
- Infections
All about Meril Life’s FIONA™
FIONA™ intrauterine device comes with an applicator that consists of a frame with a drug reservoir containing 52 mg of the levonorgestrel hormone. It releases a daily dose of 20ug of LNG into the uterine cavity. The reservoir is encased in a rate-limiting membrane that controls the release kinetics of the hormone such that the recommended dose is released daily for up to 5 years.
It reduces menstrual bleeding and cramps after the first few months of implantation, eventually causing menstrual periods to stop altogether. It may effectively relieve endometriosis and is less likely to cause side effects than high-dose progestin.
Conclusion
When seeking safe, effective, and hassle-free contraceptives, IUDs are the way to go. Though there are some potential side effects and risks, they can easily be managed with the help of your healthcare provider.