What Happens When Calcium Builds Up Inside Your Leg Arteries?
Introduction
If you have been told that there is calcium buildup in leg arteries, you may wonder what that really means. Is it serious? Is it the same as a blockage? Can it be reversed?
Calcium buildup in arteries, also called arterial calcification, is common with age. When it affects the legs, it is often associated with Peripheral Artery Disease (PAD). According to the World Health Organisation, CVD (cardiovascular diseases) accounts for nearly 27% of all deaths in India[1], and PAD is often underdiagnosed.
Understanding how calcium deposits in arteries affect blood flow can help you act early and protect your mobility and overall health.
How Does Calcium End Up in the Arteries?
You may have learned that calcium keeps your bones and teeth healthy. However, does it not belong inside your arterial walls?
Over time, you may notice that there are:
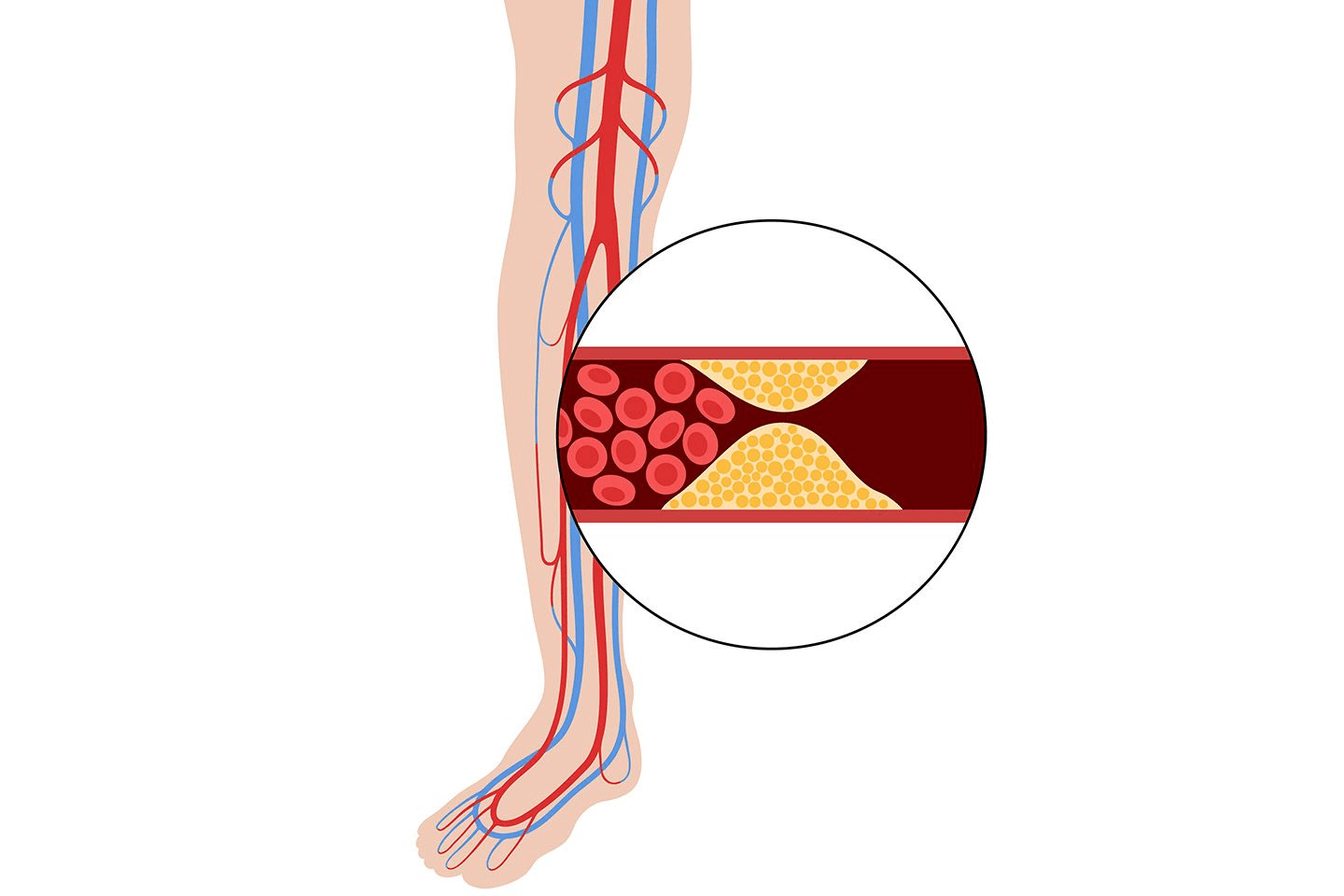
Fatty deposits, also known as plaque, build up inside the arteries
Inflammation damages the inner lining
The body deposits calcium in these damaged areas
The artery walls become stiff and thick
This process is known as vascular calcification.
Who is at higher risk?
People above 50 years
Individuals with diabetes
Smokers
Patients with high blood pressure
Those with chronic kidney disease
It is observed that arterial calcification increases significantly with age and in the presence of metabolic disorders.[2]
Is Calcium Buildup the Same as "Hardening of the Arteries"?
Not exactly, but they are closely related.
Term | What It Means |
Atherosclerosis | Fatty plaque buildup inside the arteries |
Arterial Calcification | Calcium deposition within plaques |
Hardening of arteries | Stiffening due to plaque + calcium |
Calcium makes plaques more rigid. It may reduce the artery's flexibility, making it harder for blood to flow properly. Think of it like a rubber pipe turning into a stiff plastic tube. The flexibility is lost.
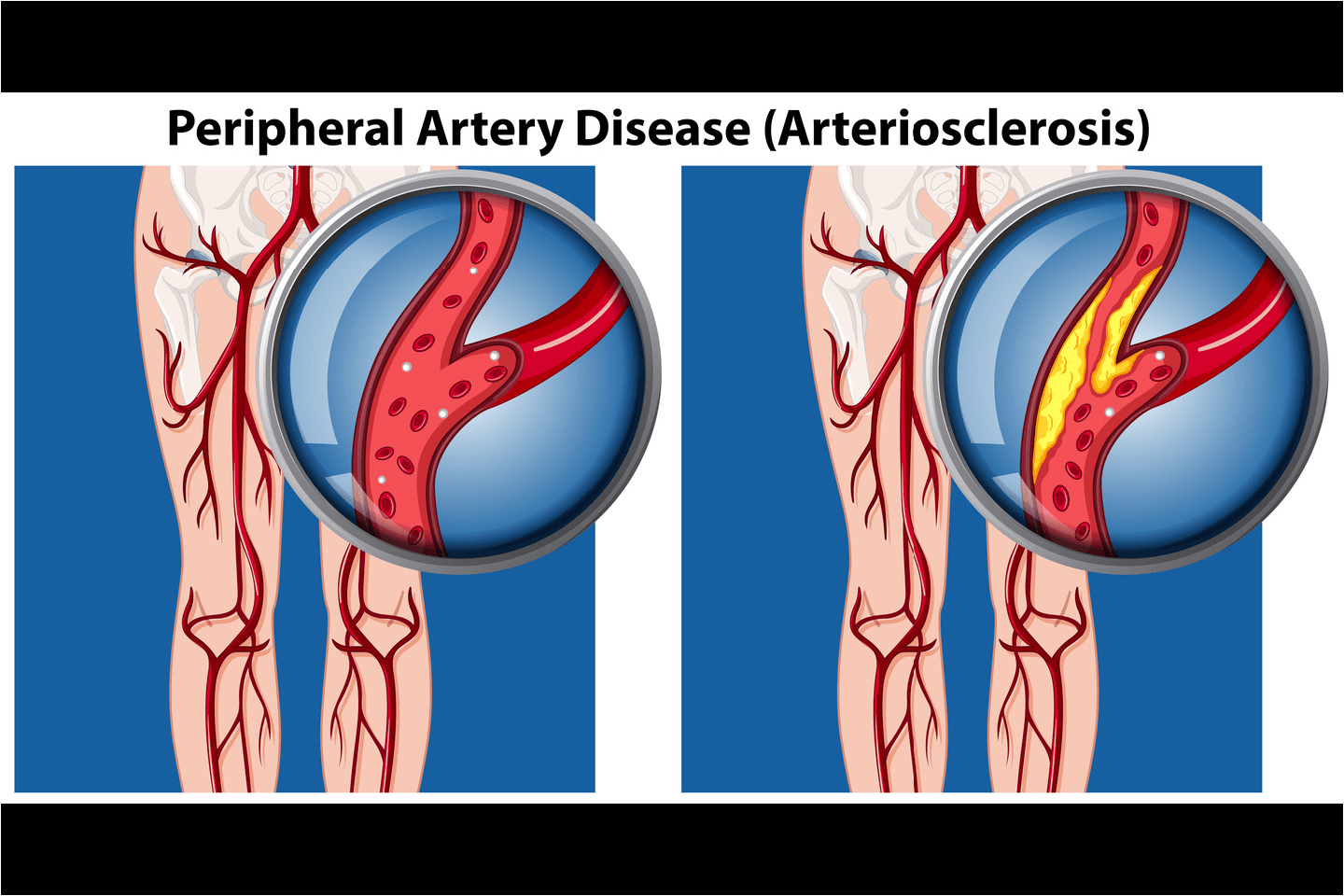
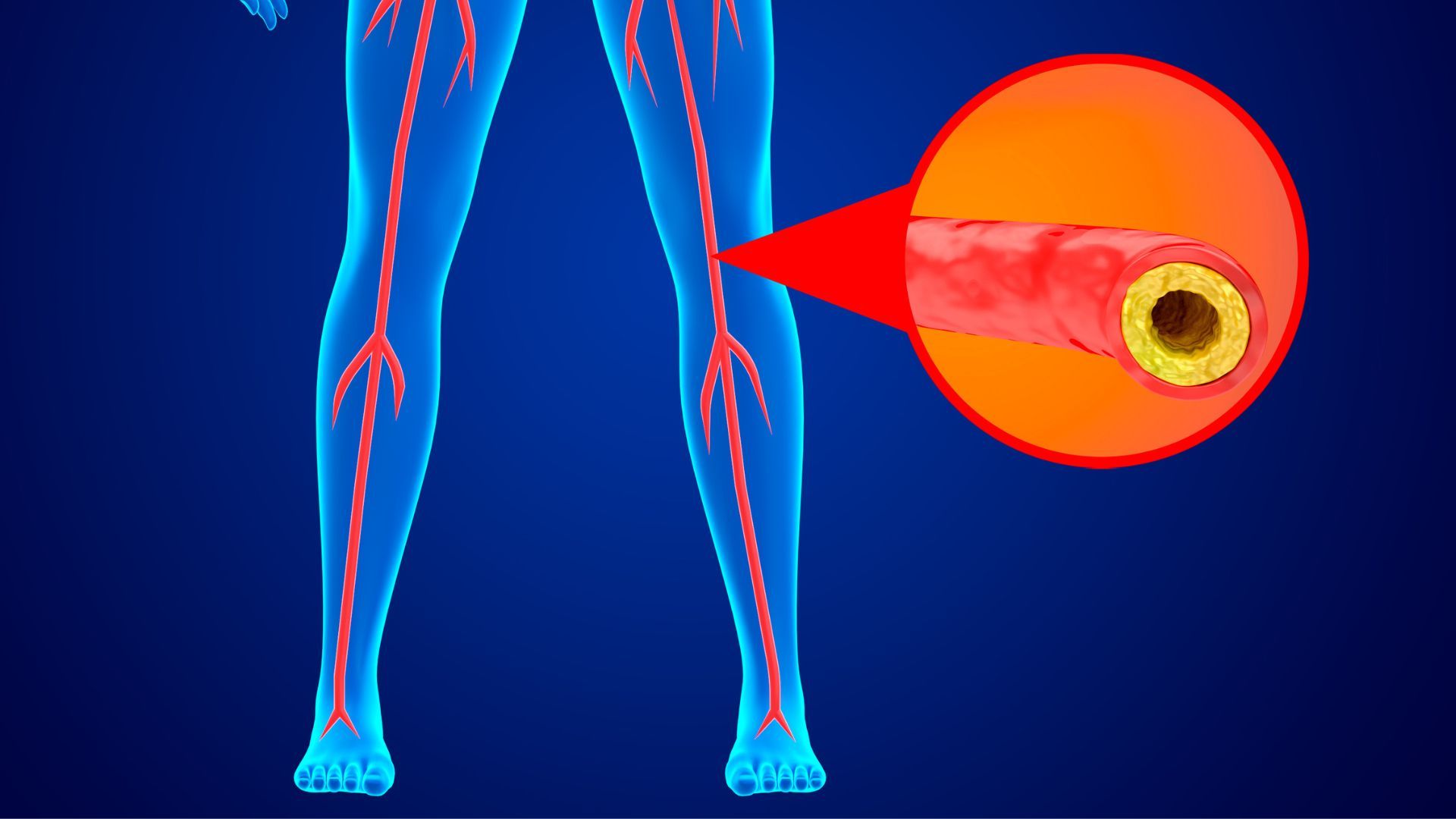
How Does Calcium Build-up Affect Blood Flow to the Legs?
Your leg muscles need a steady supply of oxygen-rich blood. When calcium narrows and stiffens arteries:
Blood supply reduces
Muscles get less oxygen
Pain develops during walking
This condition is commonly called Peripheral Artery Disease (PAD).
A review in the International Journal of General Medicine reports that PAD prevalence ranges between 20–50% in individuals with diabetes, compared to 10–26% in non-diabetics[3]. It highlights how metabolic disorders significantly increase vascular risk.
What happens inside the legs?
Narrowed arteries reduce blood flow
Walking increases oxygen demand
Pain or cramping develops
Symptoms improve with rest
It is known as claudication.
Signs and Symptoms to Watch For
You should look for early symptoms, as they may be mild and many people ignore them.
Common warning signs:
Leg pain while walking
Cramping in calves or thighs
Numbness or weakness
Cold feet
Slow-healing wounds on toes
Shiny skin on legs
Reduced hair growth on legs
In advanced stages:
Pain even at rest
Ulcers
Tissue damage (gangrene)
If untreated, severe PAD may increase amputation risk.
How Is Calcium Build-up in Leg Arteries Diagnosed?
Doctors use simple, non-invasive tests first.
1. Ankle-Brachial Index (ABI)
- When you compare the blood pressure in the ankle and arm
- Quick and painless
- ABI below 0.9 suggests PAD[4]
2. Doppler Ultrasound
- Visualizes blood flow
- Identifies narrowed areas
3. CT Angiography
- Detects calcium deposits clearly
- Shows the extent of blockage
Imaging tests help to determine the severity of calcium deposits and guide treatment. You can get an early diagnosis and significantly improve outcomes.
Can Calcium Build-up in Leg Arteries Be Treated?
Yes. Treatment depends on severity.
Lifestyle-Based Management
Smoking cessation
Blood sugar control
Regular supervised walking
Healthy diet
Medications
Antiplatelet drugs
Cholesterol-lowering medicines
Blood pressure control
Minimally Invasive Procedures
When arteries are severely narrowed, doctors may use:
Balloon angioplasty
Stent placement
Atherectomy
In complex, calcified lesions, advanced interventional systems are used to improve precision and to prepare vessels before stenting. These techniques aim to restore blood flow while minimising vessel trauma.
In very advanced cases:
Surgical bypass may be required
Treatment decisions depend on symptoms, imaging findings, and overall health.
Can Calcium Build-up Be Prevented or Slowed?
While existing calcium cannot always be removed, progression can be slowed.
Practical prevention steps:
Maintain HbA1c below recommended levels
Keep LDL cholesterol controlled
Walk at least 30 minutes daily
Avoid tobacco in any form
Maintain a healthy body weight
With lifestyle modifications, you can reduce cardiovascular risk when risk factors are addressed early.[5]
Prevention is far more effective than late-stage intervention.
When Should You See a Doctor?
Seek medical attention if you notice:
Leg pain after walking short distances
Non-healing foot wounds
Persistent coldness in one leg
Skin colour changes
People with diabetes should be especially cautious. PAD symptoms are often masked due to nerve damage.
Early consultation prevents complications.
What Can You Expect Long Term?
With early diagnosis:
Symptoms can improve
Walking distance increases
Complications reduce
Without treatment:
Your pain may worsen
The risk of infection increases
You may have to amputate an infected region
Long-term outcomes improve significantly with:
Strict risk factor control
Regular follow-ups
Adherence to medication
PAD is manageable, but it requires consistency.
Conclusion
Calcium buildup in leg arteries is not just a sign of aging. It is a marker of vascular disease that can affect your mobility, independence, and quality of life.
The good news is that early detection and lifestyle correction make a substantial difference. If you notice warning signs such as leg pain during walking, do not ignore them. Simple tests can identify the problem early. Timely care can help you stay active and reduce long-term risks.