Total Knee Replacement Surgery
Why are knees replaced with artificial implants?
Normal Knee anatomy
The knee is the largest joint in a human body and is central to nearly every routine activity. The knee is classified as a pivotal hinge joint, meaning it can straighten and bend in one direction while it allows some twisting to occur. This is known as flexion and extension; you will often hear your surgeons refer to this while discussing about your knee.
Movements at the knee joint are essential to everyday life such as walking, climbing stairs, standing and sitting. Because it is such an integral part of normal daily routine, the knee is often susceptible to injuries and arthritis.
The knee joint is formed by the ends of 3 bones:
Lower end of the thigh bone, or femur
Upper end of the shin bone, or tibia
Kneecap, or patella
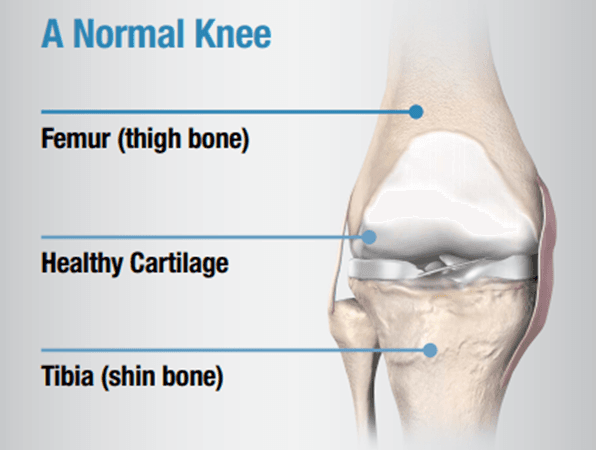
Thick, tough tissue bands called ligaments connect the bones and stabilize the joint. A smooth, plastic like lining called cartilage covers the ends of the bones and prevents them from rubbing against each other, allowing for flexible and nearly frictionless movement. Cartilage also serves as a shock absorber, cushioning bones from the forces acting between them. Finally, a soft tissue called synovium lines the joint and produces a lubricating fluid that reduces friction and thus wear.
Knee Deformities
Each patient is unique, and can experience knee pain for different reasons.
Osteoarthritis: The leading cause of knee pain is osteoarthritis (OA). OA is sometimes called as degenerative arthritis because it is a “wearing out” condition involving the breakdown of cartilage associated with the joint. When cartilage wears away, the bones rub against each other, causing significant pain, stiffness and swelling. Trauma or direct injury to the knee can also cause osteoarthritis. Without cartilage there is little shock absorption between the bones in a joint. This allows stress to build up in the bones, which further contributes to pain.
Rheumatoid Arthritis: Another common cause of knee pain is rheumatoid arthritis (RA). RA produces chemical changes in the lining of the joints, or synovium, which causes it to become thickened and inflamed. In turn, the synovial fluid destroys cartilage. The end result is cartilage loss, pain, and stiffness.
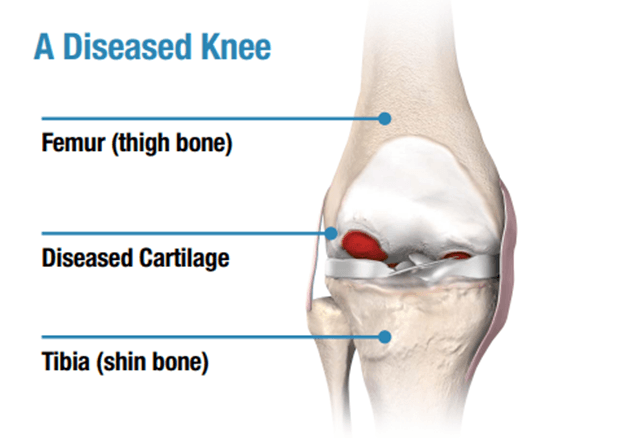
Depending on your specific diagnosis, the doctor may recommend conservative treatment options like bracing, medication, joint fluid supplements or physical therapy. However, if you haven’t experienced adequate relief with these conservative treatment options, your doctor may recommend total knee replacement which may provide relief from arthritis pain and enable you to return to your normal activities.
When is knee replacement needed
Arthritis pain can begin suddenly, but it is most likely to develop gradually over a period of time. You may first experience pain while waking up in the morning or when you stand up after sitting for a while. Some patients say changes in weather can bring on arthritis pain. Eventually you may notice that the pain has taken over your ability to complete everyday tasks. It may hurt to walk, climb stairs, or even sit down. You may not be able to bend or straighten your knee as you once could. You may also feel a grinding sensation in your knee or popping and cracking sounds when you walk. Arthritis can even wake you up in your sleep. The appearance of your knee may change and become deformed due to the breakdown of the joint.
Knee replacement surgery is considered, once all other conservative options have failed to provide any relief. If you have tried all your doctor’s recommendations and are still experiencing pain, stiffness, or lack of stability, then it is the time to consider making a choice that will allow you to get your life back. There may come a time when knee replacement is the only treatment option. The decision to have a knee replacement surgery is made with your surgeon and is based on your general medical health and how much your daily life is affected by your knee:
Pain – affects your activities of daily living, your walking, or even sleep
Swelling – does not improve with rest or medications
Stiffness – inability to bend or straighten the knee
No improvement with medications, therapy, or knee injections
Degree of deformity
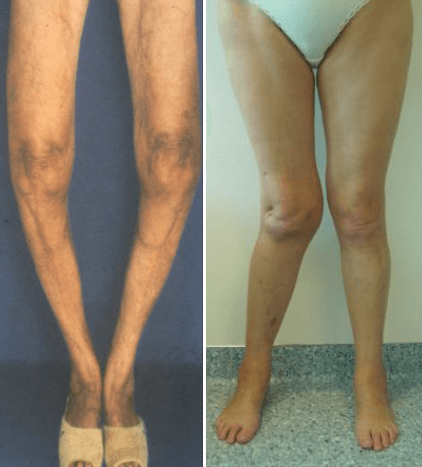
Varus & Valgus deformities
What does total knee replacement / arthroplasty mean?
Knee replacement surgery is also called as arthroplasty and this procedure involves removing parts of the damaged knee and replacing them with artificial parts called prosthesis.
Your orthopedic joint replacement surgeon will remove the damaged and diseased portions at the end of the femur (thigh bone) and top of tibia (shin bone) and replace them with artificial implants made up of metal or plastic. Each bone is shaped to exactly fit the prosthesis. Components are then attached to the thigh bone, shin and knee cap, most commonly using surgical cement. The surgeon may need to resurface the back of the kneecap, known as the patella.
The artificial prostheses consist of three pieces:
Femoral component – metal piece that caps the end of the femur and has a groove, which allows the kneecap to move up and down as the knee bends and straightens
Tibial component – flat piece of a metal with a plastic plate that covers the top of the tibia.
Patellar component – dome-shaped piece of plastic that allows it to glide
Diagnosis:
Physical examination: Medical history, symptoms, and level of pain, muscle strength, joint motion, and knee alignment. Blood tests and other laboratory tests
Radiographic Evaluation: X-rays, Magnetic Resonance Imaging (MRI)
What are the goals of Total knee replacement (TKR)/ Total knee arthroplasty (TKA)?
The following are the clinical goals of a Total Knee Replacement(TKR) procedure
To put the implants in a correct alignment and position
To ensure that the remaining soft tissues are balanced
To ensure that the implant is well fixed to the bone
To ensure that the implant used is designed to offer high level of function & longevity
The above clinical goals translate to the following qualitative goals from a patient standpoint
To relieve pain
To restore function
To last as long as possible
How is knee replacement done- An Overview
When the decision is made to perform a total knee replacement, your orthopedic surgeon will require a few activities to be completed prior to knee replacement surgery that may include the following:
Complete Physical Examination: Your doctor will ask for an examination as well as some tests to be completed such as blood work, an EKG, and a chest x-ray.
Surgical Consultation: Your doctor will review the procedure with you and answer the questions if any. You will need to sign a surgical consent form. Doctor will also review the test results from your physical examination and you will notify the surgeon of any allergies or medications you currently take.
Patient preparation for Knee surgery:
Consumables used in this step include (but not limited to) bandage / drape for wrapping patient’s legs, leg positioning tools and anesthesia for the patient.
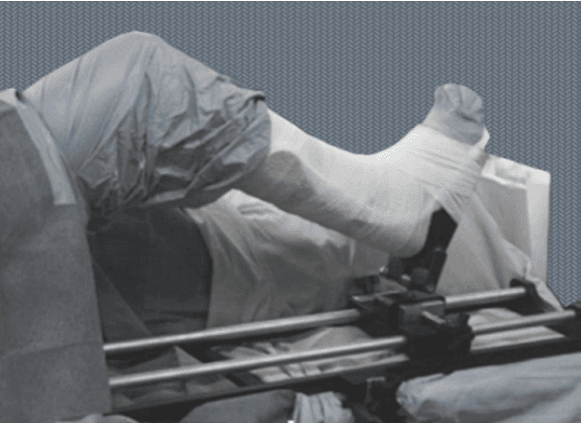
Supine positioning on the OR table
Pneumatic tourniquet is used (high up in the thigh) to minimize blood loss during surgery
Special table support may be used to allow the knee to be flexed and extended several times during the procedure
Required levels of anesthesia (general anesthesia) are given to the patient
Alignment of the axes
In a normal knee, there are two axes:
Mechanical axis: this is a straight line that connects the femoral head, passes through the knee and the center of the ankle joint.
Anatomical axis: this is a straight line that passes through the bone shaft of the femur as well as the tibia
On the femoral side, there is 5-7 degrees of angular difference between the anatomical axis and the mechanical axis, whereas the axes are parallel on the tibial side.
In a deformed knee these angles deviate from the nominal values and hence bone cuts have to be made at specific angles in order to achieve appropriate alignments on the femoral as well as tibial side.
This is one of the critical goals of the Total Knee replacement procedure and hence several precision instruments are provided that produce artificial prostheses in order to enable the surgeons to measure the deviations and plan for appropriate cuts to achieve alignment between the axes and the components.
Overview of femoral and tibial cuts in Total Knee Replacement-The surgeon goes through the following bone cuts on the distal femoral end and proximal tibial side once the appropriate plan is made based on the axes alignments.
Transverse distal femoral cut
Medial/lateral femoral jig location
Anterior femoral cut
Posterior femoral cut
Anterior and posterior femoral chamfer cuts
Transverse proximal tibial cut
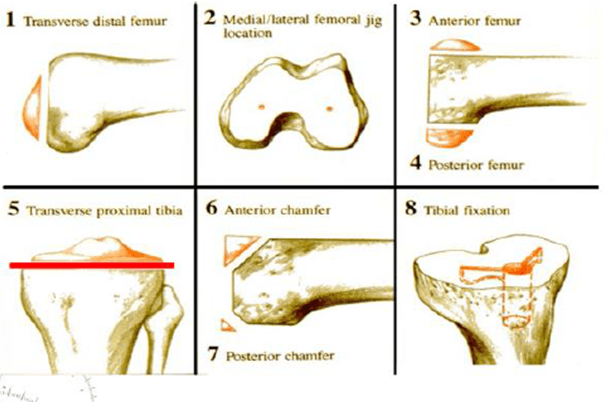
Note: All surgeons do not follow the exact sequence of cuts listed above. They differ based on their preferences and surgical training.
There are 2 surgical techniques which the surgeons follow
- Posterior referencing
- Anterior referencing
and based on these techniques, the instrumentation is used.
Overview of implanting of prosthesis in Total Knee Replacement
Once the satisfactory cuts are made and the trailing is done, the actual components (Femoral component, tibial component and poly liner) are fixed with the help of bone cement.
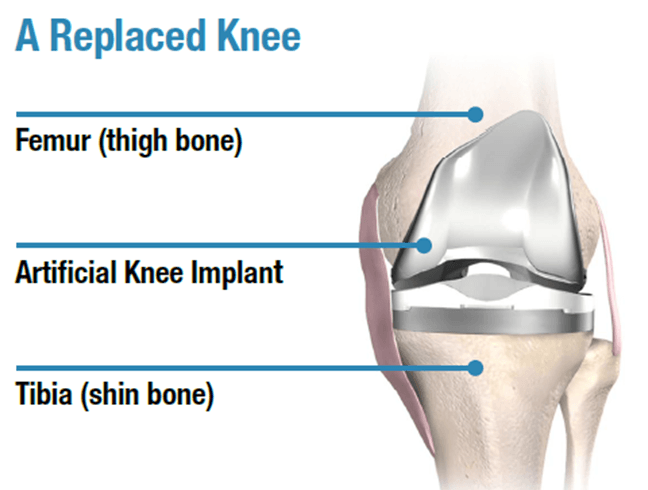
Total knee REPLACEMENT surgery - Post-Operative Care/ rehabilitation
Once the knee surgery is completed, the patient will be transferred to a room for close observation of vital signs, circulation, and pain management. Once the patient is awake, you may notice the following:
A drain near incision to collect the drainage and monitor its amount
Elastic hose or compression stockings to help minimize the risk of blood clots
Bandage covering the incision area to maintain cleanliness and prevent infection
Pain pump to manage pain levels
Catheter inserted into your bladder
Ice packs to reduce the swelling in knee area
You can expect to be up on your feet within a day. That might be hard to do on your own at first. So you may need parallel bars, crutches, a walker, or a cane for a while.
Usually, you can expect a big improvement in flexibility and much less pain within a month. It is important to exercise your knee often; initially you will need help of physiotherapist to keep down swelling and to strengthen your muscles.
One of the first priorities is to get your new knee moving – to regain the range of motion.
Following total knee replacement surgery, patients are encouraged to resume an active lifestyle.
Meril Knee Implants
Meril orthopaedic products are used in more than 50 countries restoring their mobility to suit their lifestyles and thus adding more to life, globally. Meril is committed to lead innovation by developing a strong pipeline, patient centric innovative products to offer in future.
The FREEDOM ® Total Knee System was developed using advanced design engineering technologies and extensive clinical experience to address the anatomical, physiological and lifestyle needs of today's patients. It provides high-flexion and is a USFDA-approved and CE-certified knee implant

