8 Different types of colon resection surgery options
Colon Resection Surgery Explained
The intestine – a long tubular organ comprises of the small intestine, the large intestine, also known as the colon, and the rectum. The rectum is the last part of the colon. Once the food is swallowed, it starts digesting in the stomach and gets emptied in the small intestine. The small intestine absorbs the nutritional elements of the food. The remaining waste then moves from the colon to the rectum, until it is ultimately expelled from the body. The colon and the rectum continue to absorb the water and hold the waste until one is ready to expel it. As one grows old, the colon may start developing problems and may need treatment to prevent conditions and diseases that can affect it. In such a situation, one may need a colon resection surgery. Let's understand what it is, its types, why it may be required and more.
What is colon resection surgery?
A colon resection surgery, also known as colectomy, is one of the different types of surgeries that help treat colon diseases. When one undergoes a colon resection surgery, the surgeon removes either a portion of the colon or the entire colon. After removing the diseased portion of the colon, the surgeon connects the remaining healthy parts through a procedure known as anastomosis.
A patient may need to undergo a colectomy to treat diseases like colon cancer and diverticulitis, i.e. the inflammation of a diverticulum (the small, bulging pouches forming in the digestive system's lining in the colon). Diverticulitis causes acute pain and disturbance of the bowel function.
Types of colon resection operations
The following are some of the types of colectomy operations
- Total colectomy in which the surgeon removes the entire colon.
- Partial or subtotal colectomy in which the surgeon removes only a part of the colon.
- Hemicolectomy in which either the right or the left portion of the colon is removed.
- Proctocolectomy in which the surgeon removes both the colon as well as the rectum.
- Proctectomy in which the rectum is removed.
- Segmental colectomy in which the diseased segment of the colon is removed
- Low anterior resection in which the sigmoid colon and upper rectum is removed.
- Abdominoperineal resection: In which the sigmoid colon, rectum and anus are removed.
Preparing for a colon resection procedure
In case of a scheduled colon resection, the surgeon may ask you to do a few things at home in the days leading up to your surgery.
- You may be asked to stop taking medications, especially a few specific ones that can increases complication risks during the surgery.
- Your doctor may ask you fast for a specific number of hours before your surgery.
- The doctor may also prescribe a laxative solution to clear your bowels. You need to mix the solution with water and drink at home. You will be told when to drink it. Note that the solution causes diarrhoea, so that the colon is emptied before the surgery.
- It is also possible that the doctor may prescribe antibiotics. The antibiotics help suppress the naturally found bacteria in the colon and help prevent infections.
Note that the above preparations are possible only in case of a scheduled procedure. Sometimes patients need to undergo an emergency procedure, which leaves them with no preparation time. For instance, if a patient needs an emergency colectomy due to bowel perforation or bowel obstruction, it may not leave them any time to prepare for the surgery.
Undergoing colon resection- the two types of surgeries
Before you undergo the colon resection surgery, the doctor will monitor your breathing and blood pressure. You may also be given an antibiotic medication injection. The surgeon then administers anaesthesia before proceeding with the colectomy, which may be performed in one of the two ways:
Open colectomy
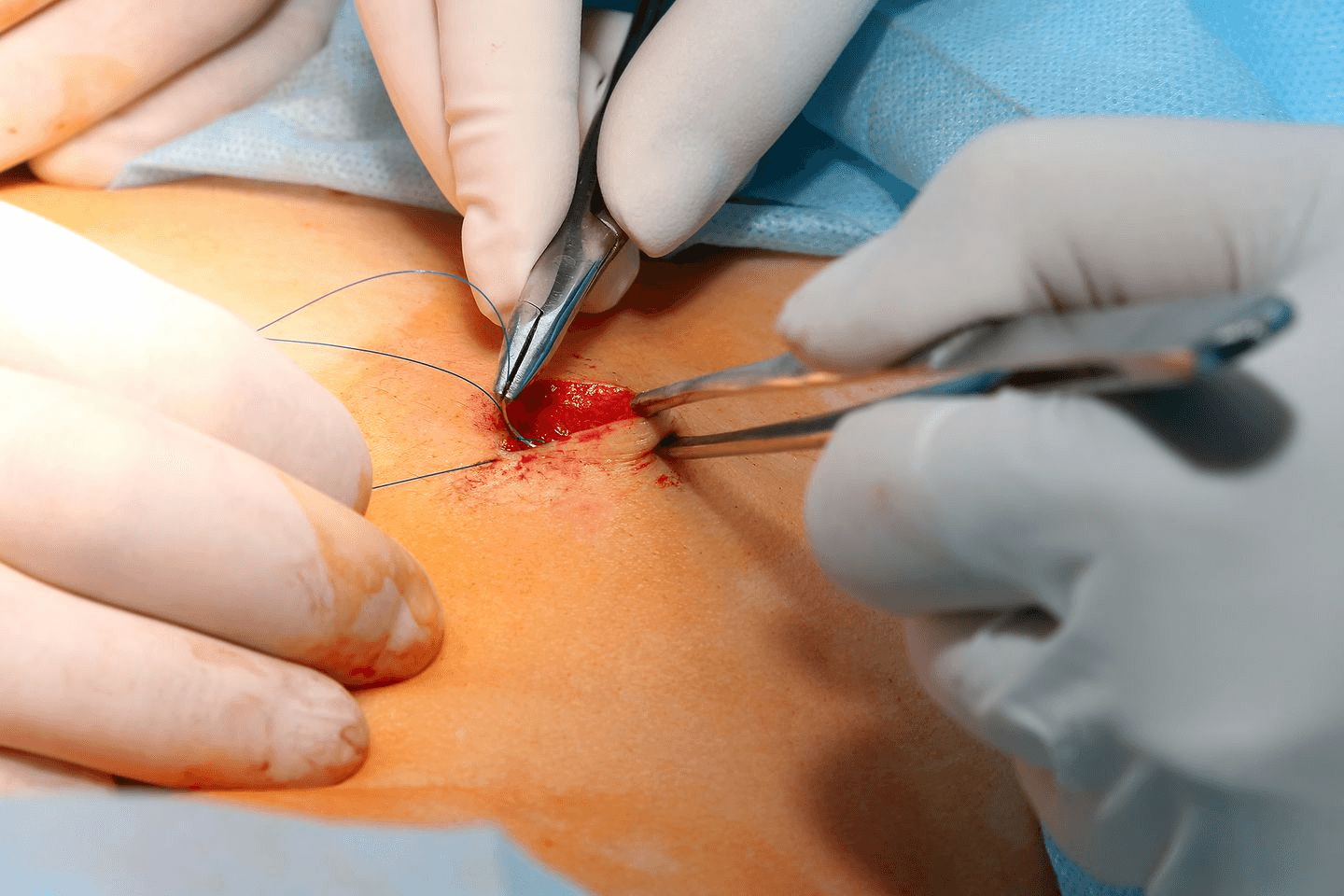
An open colectomy, simply known as open surgery, is when the surgeon makes a longer incision into your abdomen to access your colon. The surgeon then uses the necessary surgical tools to free your colon from surrounding tissues, and cuts out the colon partially or entirely, as needed.
Laparoscopic colon resection
The second type of colectomy is known as the Laparoscopic colon resection. The minimally invasive laparoscopic colon surgery allows the surgeon to perform various standard colon procedures by making a small incision.
During a laparoscopic colon resection, the surgeon operates through four or five small openings (each of which is approximately a quarter-inch). The surgeon passes a small video camera through one of the incisions, while special surgical tools are passed through the other incisions. A video screen is placed in the operating room, on which the surgeon watches an enlarged image of the internal organs of the patient. The surgical tools passed through the incision help free the colon of the surrounding tissue, thus enabling the surgeon to operate on the colon, outside of the patient's body. Once the colon is repaired, the surgeon reinserts it through the incision.
Meril’s Mirus Linear Cutter is a reloadable linear cutter and reloads are available in lengths of 60mm, 80mm and 100 mm with two different sizes of staples to accommodate various tissue thicknesses and has applications in has application in gastrointestinal, thoracic, and pediatric surgery for transection, resection and anastomosis.
Selecting the procedure and post colectomy options
Whether a patient needs to undergo an open colectomy or a laparoscopic colon resection surgery depends on the patient's situation and the surgeon's expertise. While a laparoscopic colectomy reduces the pain and enables the patient to recover more quickly, it may not be suitable for every patient. Sometimes a surgeon may begin the laparoscopic procedure but may need to convert it to an open colectomy.
Upon repairing and removing the colon, the surgeon reconnects the digestive system to allow the body to expel the waste, using one of the procedures mentioned below:
Rejoining the remaining portions of the colon
Once the colon is repaired, the surgeon may either attach it to the small intestine or stitch the colon's remaining portions together (anastomosis). This allows the stool to leave the body as before.
Meril’s MIRUS™ Circular Stapler is a sterile single patient use, mechanical instrument design reflects three decades of experience drawn from leading Bariatric, Colorectal and General Surgeons across the globe. With consolidating exclusive technology,4.5 mm staples and other unique features ,the MIRUS Circular Stapler gives phenomenal clinical performance, usability and adaptability
Connecting the intestine via an opening created in the abdomen
Here, the surgeon attaches your large intestine or colon to the small intestine by creating an opening in the abdomen, allowing the waste to leave the body through the opening, known as a stoma. The surgeon may attach a temporary or permanent bag on the outside of the stoma where the stool is collected.
Connecting the small intestine to the anus
If the surgery requires removing both the patient's colon and rectum, the surgeon typically uses a portion of the small intestine to create a pouch attached to the anus. This allows the patient to expel the waste naturally. A side effect of the colectomy procedure is that the patient may experience several watery bowel movements.
What to expect Post colectomy
Immediately after the surgery, the patient is moved to the recovery room and monitored until the effect of the anaesthesia wears off. The patient is then moved to the hospital room, where they can continue with the recovery. Typically, patients are asked to stay in the hospital until they regain their bowel movement, which may take a couple of day to a full week.
In the first few days of the surgery, patients may be unable to eat any solid foods and maybe prescribed liquid intravenous nutrition, usually in the arm. They are then allowed to drink clear liquids. Patients can eventually start adding solid foods to their diet, once their intestines recover.
For patients who had to undergo a colostomy or ileostomy in which the intestine is attached outside the abdomen, an ostomy nurse will explain to such patients how they need to care for the stoma. The nurse explains how the stoma bag collects waste and how to change it.
It typically takes a couple of weeks for patients to recover from the colon resection surgery, but recovery can begin at home. While patients may feel weak at first, they will gradually regain their strength.
Risks associated with colon resection
The following are some of the common risks associated with colon resection surgeries:
- Reactions to anesthesia
- Internal bleeding
- Blood clots in the lungs or legs
- Hernia
- Infection at the site of the skin incision
- Damage to nearby organs
- Stomach Infection
- Leakage on the site where intestines are sewn together
- Scar tissues in the stomach that can block the intestines
Post-surgery consultations
Typically, patients are asked to go for a follow up a few days after the procedure. However, patients should consult their doctors immediately in case:
- They are suffering from a fever of 100.4°F or higher
- They notice redness, bleeding, swelling or fluid leakage from the incision
- They experience shortness of breath
- Their pain gets worse
Final note
A colon resection surgery is a painless surgery since it is performed under general anesthesia. However, patients may feel abdominal pain, typically due to the incision. However, pain can be managed with medication. Consult your doctor about the risks associated with the surgery and the post-surgery treatment and care required, if any.