Drug Eluting Stent: What is It & How It is Implanted? | Meril Life
Overview of Drug-Eluting Stents
When the coronary arteries become narrowed due to plaque build-up, it results in a condition known as coronary artery disease or CAD. CAD is a critical condition as it can interrupt the blood flow to the heart muscles. Heart muscles that do not receive sufficient oxygen-rich blood can become damaged, putting the patient at higher risk of suffering a heart attack. As such, patients with severe coronary artery disease are typically advised by their interventional cardiologist to undergo stent implantation to treat the condition, or in some cases referred to a cardiac surgeon to undergo bypass surgery. The interventional cardiologist performs a procedure known as coronary angioplasty, in which a stent is inserted into the patient's coronary artery. Today, most medical practitioners recommend drug-eluting stents as opposed to bare metal stents to their patients. Let's understand what it is, along with the components and procedure of implanting the stent. We shall also examine drug-eluting stent benefits and risks.
What is a coronary drug-eluting stent?
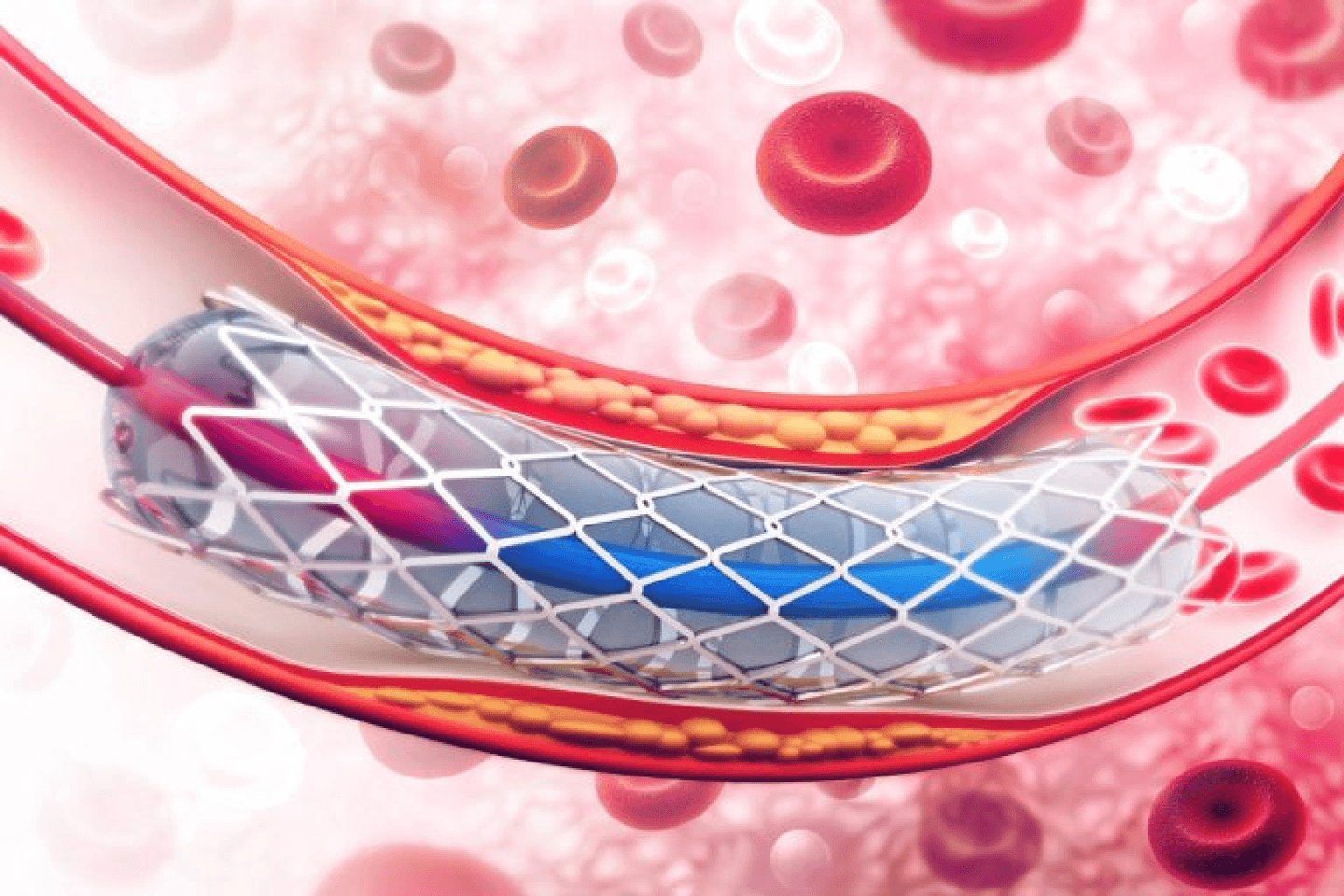
A stent is a tiny, metal mesh tube or a scaffold-like device designed to support the artery walls and prevent plaque from blocking the blood flow. Once the doctor implants the stent in an artery, the blood flows more freely to the part of the patient's heart which that artery was supposed to supply blood to. A drug-eluting stent or DES is a metal stent coated with a pharmacologic agent or drug. This type of stent is known for suppressing restenosis, i.e. the closing up or re-blocking of an artery after an angioplasty as a result of excess tissue growth at the edge of or inside the stent. In modern practice, most patients are treated with such drug eluting stents.
Comparing coronary drug-eluting stents to and bare-metal stents and simple balloon angioplasty without a stent:
As per a study conducted by the American Family Physician medical journal, approximately 40% of people who underwent angioplasty without a stent experienced restenosis. The figure dropped to around 30% for patients who opted for a bare-metal stent. It further dropped to less than 10% for people who opted for drug-eluting stents.
Components of drug-eluting stents
Coronary drug-eluting stents have three major components. They are as follows:
- The metal stent structure
The first component is the metal stent structure, which is also referred to as the stent platform. It is generally made of either surgical stainless steel or some alloy such as cobalt-chromium
- The polymer
The second component is the polymer that coats the metal stent. This coating contains the drug and slowly elutes (delivers) it to the arterial wall over time.
- The drug itself
The drug is the final component of the DES. The drug suppresses any excess tissue formation, which is sometimes known as scar tissue. Some commonly used drugs are Sirolimus, Zotarolimus, Everolimus, Paclitaxel, etc.
Drug-Eluting Stent Implantation Procedure
- The decision-making process
To ensure long-lasting success and optimal placement of a drug-eluting stent, the interventional cardiologist makes several important decisions while choosing and placing the stent. The operator examines the correct size of the stent length and diameter to match the lesion's (blockage) length and artery's diameter respectively. Personal factors of the patient, such as their age, weight, lifestyle, and health conditions, are also considered in the decision-making process. - Preparing for the DES procedure
An interventional cardiologist inserts the drug-eluting stent into the patient's coronary arteries in a coronary angioplasty procedure. The procedure is usually conducted after administering local anaesthesia to the patient. Depending on the severity of the patient's condition, it can take thirty minutes to several hours to complete the procedure. - The procedure
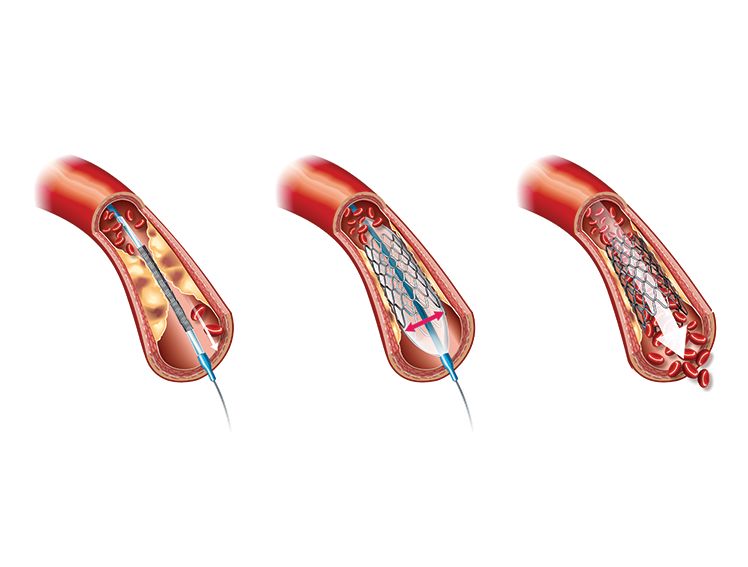
To begin the procedure, the interventional cardiologist first makes a small incision into the patient's arm or groin. A small catheter with a balloon and stent is inserted on the tip into the incision. The operator then uses special dyes along with sophisticated imaging techniques to guide the catheter through the patient's body and into the narrowed coronary artery. After this, the operator inflates the balloon in order to widen the artery and radially push aside the plaque build-up. As the balloon inflates, it will also expand the stent, which once deployed does not collapse, holding the artery open. The operator then removes the balloon and catheter, and the stent is left behind.
How the DES works
Once the operator inserts it, the drug-eluting coronary stent begins to release medication directly into the patient's artery. The medicine-coated stent helps prevent the formation of scar tissue within the stent. It also prevents the narrowing of blood vessels.
Post-Procedure Care and Recovery
The doctor may also prescribe some additional medication after the procedure, including blood thinners. The patient may be asked to stay in the hospital overnight to monitor for any adverse side-effects. As the patient begins to recover, the stent's artery begins to heal. The now open artery allows proper blood flow to the heart, leading to immediate improvement in the way the patient feels. To ensure optimum effectiveness, the patient must take the prescribed medication. They must immediately consult the doctor upon experiencing discomfort.
Maintaining Heart Health After DES
After undergoing the DES insertion procedure, the patient must take the necessary steps to reduce further instances of heart diseases. As such, they must control their blood pressure and cholesterol levels and ensure they maintain a healthy weight. Patients can significantly reduce the risk of heart attacks and of developing blocked arteries by practising healthy habits. For instance, the doctor may advise the patient to follow a healthy, nutritious diet and include mild exercises like walking for 30 minutes daily. Adopting a healthier lifestyle also means that the patient may be asked to quit smoking or cut down on the consumption of alcohol.
Benefits of Drug-Eluting Stents
Let us now examine the benefits of a drug-eluting stent.
- DES helps prevent plaque build-up
Coronary drug-eluting stents are now the norm when treating CAD, with the drug coating ensuring an avoidance of restenosis at the lesion site. - Minimally invasive procedure
The procedure of inserting the DES is much less invasive as compared to a coronary bypass or an open-heart surgery, and is typically recommended for patients who would be too frail to undergo a heavily invasive procedure like a bypass surgery. - Quicker recovery period
Most patients undergoing the DES implantation procedure recover within a few days and can resume their normal activities within a week or two. In comparison, people who undergo coronary bypass surgery may take a more extended recovery period of six or more weeks to return to their normal activities. If the bypass surgery involves a sternotomy (where the breastbone is cut open to access the heart and then rejoined), the full recovery to normal activity can take a long time.
Meril’s Drug-Eluting Stents
Meril’s EVERMINE50 is a DES with ultra-low strut thickness of 50μm that promotes early vascular healing. The science is well established that thinner have better long term outcomes, and the 50 micron stent from Meril is the thinnest commercially available stent in the market right now. The stent is coated with a biodegradable polymer carrying Everolimus drug which is proven clinically safe and efficacious. Meril also offers BioMime™, a Sirolimus Eluting Coronary Stent System with an ultra-thin (65 µm) strut thickness. Both Evermine50 and BioMime™ contain a novel hybrid cell design with closed cells towards the ends and open cells in the middle for adequate side branch access and uncompromised radial strength.
Risks of Drug-Eluting Stent Implantation
All procedures come with some risk. Just as it is essential to analyse the drug-eluting stent benefits, so is it critical to consider its risks, though such eventualities are rare. Here are some of the risks associated with DES insertion procedure.
- Patients may have an allergic reaction to the anaesthesia, dyes, drug in the coating, and other materials used in the procedure
- The dye used in the procedure may be detrimental to the kidney
- Patients may experience bleeding or clotting after the surgery
- Insertion site infection.
- Patients may experience abnormal heart rhythms, also known as arrhythmia
- While it is very rare, there are chances that the patient may suffer a heart attack or a stroke
The doctor typically informs the patient of all the risks and side-effects of stent insertion, and all precautions are taken to ensure a successful procedure. It is recommended that the patient consult the doctor on what to expect post procedure and report issues immediately upon noticing any abnormalities. Patients must also immediately inform the doctor if they experience any chest pain, as it could indicate serious complications.
Final note
Cardiology as a field has been advancing with every passing year. Coronary drug-eluting stents are one of the newest advances and considered a breakthrough in the field of interventional cardiology. Today, there are different types of drug-eluting stents available in the market. If you need to undergo a stent placement procedure, speak to your health care provider about the drug-eluting stent benefits, its suitability to your specific clinical conditions and expected efficacy of the procedure for you.