Risks involved in scheduling C-section after 35
Why a scheduled C-section after 35 might be too risky?
A Cesarean delivery proves to be a useful intervention for expectant mothers in many situations. Today, many pregnant women, request their gynaecologists to help them plan or schedule their deliveries on their preferred dates. Similarly, working women prefer to coordinate their work schedules with their maternity leaves. With more and more women are opting to have only one child, usually later in life, scheduled C-sections have become rather common. While science makes almost everything possible, scheduled Cesarean deliveries for geriatric pregnancies can have potentially adverse consequences on both, maternal as well as neonatal health. Here are some reasons why a Cesarean delivery after 35 might prove to be risky.
Understanding The C-section procedure
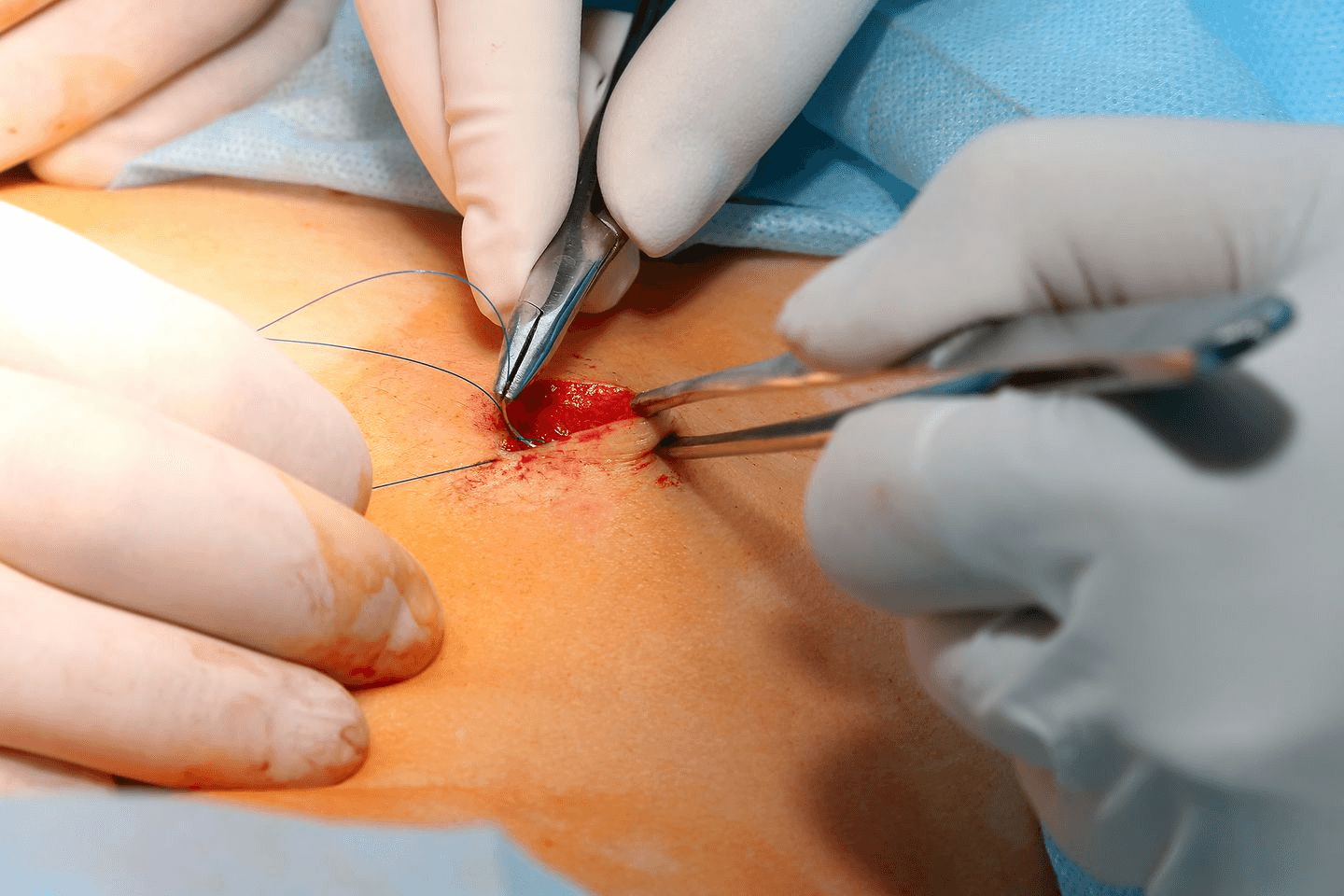
In the C-section procedure, anaesthesia is administered to the mother. The surgeon makes a horizontal incision above the pubic hairline, across the pelvis. In case of emergency C-sections, the incision may also be vertical. After the incision is made, the surgeon makes a second incision into the uterus, from which the baby is removed.
After tending to the baby, the doctor repairs the uterus using dissolving stitches and closes the abdominal incision with sutures. Meril’s MITSUTM Polyglactin 910 Suture is used in C-section deliveries. MITSU is a mid-term absorbable braided and coated synthetic suture made of poly (glycolide-co-l-lactide) (90/10). MITSU™ degrades by hydrolysis and assures predictable and reliable absorption. It is available in a broad range of suture sizes and lengths, and comes as a pack with standard stainless steel needles of different types and sizes. MITSU™ complies with the “Absorbable Surgical Suture” requirements as per the United States Pharmacopeia (USP) and “Sterile Synthetic Absorbable braided strands” requirements as per the European Pharmacopeia (EP).
The CMAJ study – Background
A Cesarean delivery typically carries more risk over vaginal birth, irrespective of the expectant mother’s age. While this is common knowledge, a study published by the Canadian Medical Association Journal (CMAJ) in 2019, suggests that the risk of scheduling C-sections for advanced maternal pregnancies is quite skewed.
As per the report by CMAJ, 1 out of 5 women in developed countries is opting for C-section deliveries over normal deliveries. According to the study, women over 35 years of age, in general, are at more significant risks of maternal morbidity as compared to younger women. The stakes are heightened for women over 35, opting for Cesarean delivery. Such women may suffer from a wide range of delivery-related complications.
The CMAJ study and risk profile
In a bid to get a clearer picture of complications associated with pregnancies, CMAJ researchers examined data on 1,444 women who experienced severe complications after delivering their babies. These complications were unrelated to their pre-existing health issues. The researchers further examined 3,464 women who did not face any difficulties.
Post-delivery Complications
As per the study findings, women who opted for Cesarean delivery were 80% more likely to suffer from complications than those who opted for vaginal deliveries. Women over the age of 35 who opted for cesarean deliveries were almost three times more likely to suffer from severe complications. With age, a woman’s uterine muscle starts losing its ability to contract efficiently, contributing to obstetric haemorrhage or severe bleeding among older women after undergoing a C-section. As per the study, 85.3% of the complications involved obstetric haemorrhage after delivery. According to Dr. Robyn Horsager-Boehrer, M.D. Obstetrics & Gynecology of UT Southwestern Medical Centre, women over 35 years, opting for C-sections are also at risk of stroke, blood clots in the lungs, liver, kidney, and cardiac dysfunction, as well as admittance into intensive care units.
C-sections performed after expectant mothers went into labour
As per the CMAJ study, women of all age groups had increased complication risks with cesarean delivery which were performed after the expectant mother went into labor. Such a decision is typically made due to medical issues arising in women, or for the babies' sake, leaving mothers with no choice but to schedule a C-section. Mothers under the age of 25 years undergoing C-sections post labour due to pregnancy complications, were 60% more likely to have post-pregnancy complications than those who opted for vaginal births. However, the figures are a lot more alarming for women over 35 having to undergo scheduled C-sections after going into labour or due to complications. The CMAJ study assessed that such women were four to five times more likely to suffer from complications as compared to women over 35 opting for vaginal births. However, for C-sections scheduled before going into labour, the risk of complications was noticed only in the oldest women, i.e. women opting for scheduled C-section after 40 years old.
CMAJ study- Intension and conclusion
It should be noted that the CMAJ study was not a controlled experiment designed to compare C-sections and vaginal births and the complications arising from them. It also did not intend to determine how the timing of the surgeries at the start of labour may impact the risk. Furthermore, CAMJ researchers have acknowledged that they could not account for every pre-existing health condition of the expectant mothers or the complications that resulted in them opting for a Cesarean delivery.
Despite this, the results indicate that women need to be extra cautious while scheduling C-sections unless they are absolutely sure of its necessity. The risk of a Cesarean delivery accumulates over the lifetime of the woman. A first C-section increases the risk of a c-section for subsequent pregnancies, leading to further complications. C-sections could also affect a woman’s ability to get pregnant again in future. As such, women should be judicious in their decision of opting for C-sections, irrespective of their age.